Dupilumab, a targeted biologic therapy widely used in moderate-to-severe atopic dermatitis, has been associated with certain cutaneous adverse effects, most notably facial redness. This phenomenon has been increasingly linked to a possible immune response to Malassezia, a common skin yeast. While antifungal agents such as itraconazole, fluconazole, and ivermectin have shown benefit in managing facial erythema, reports of similar reactions affecting the palms remain scarce.
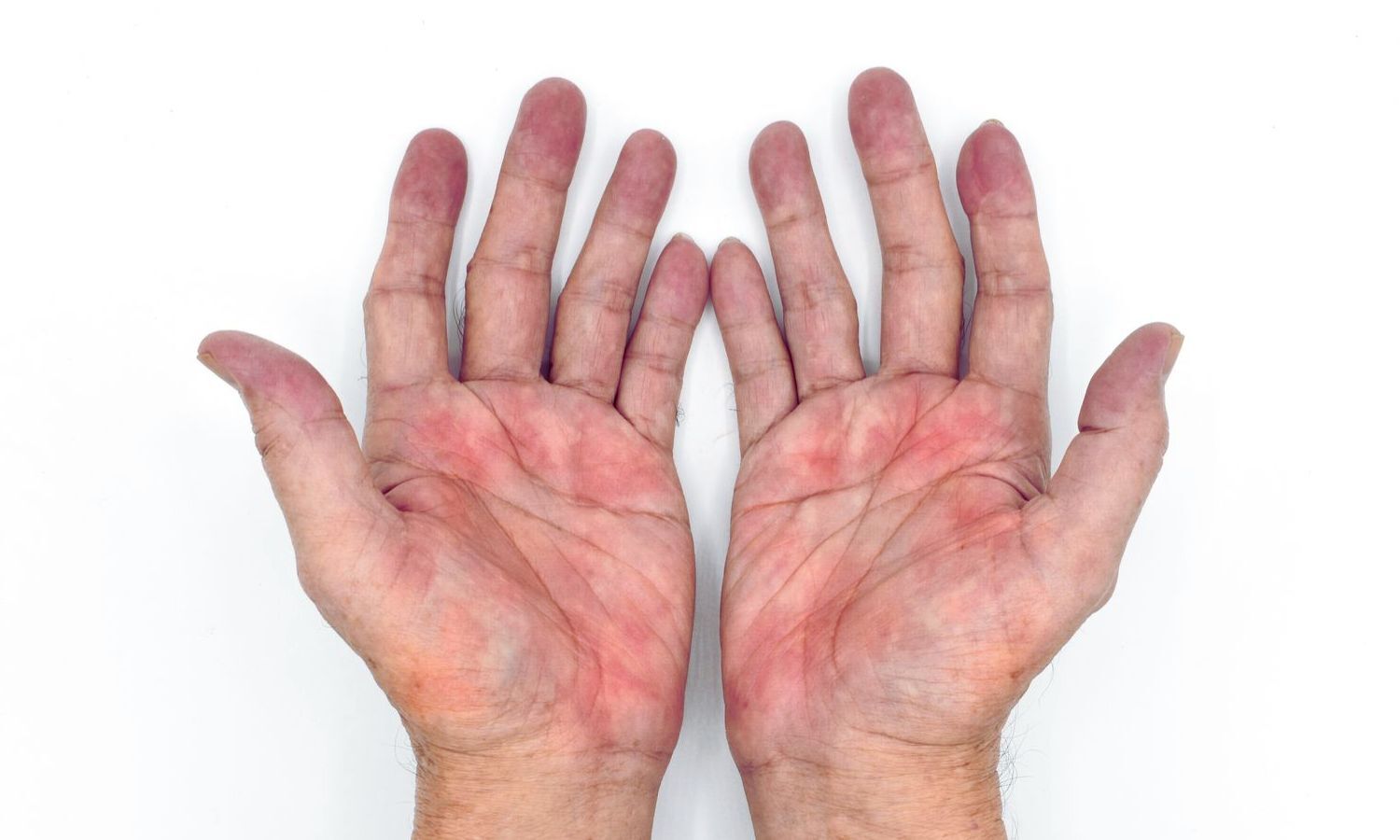
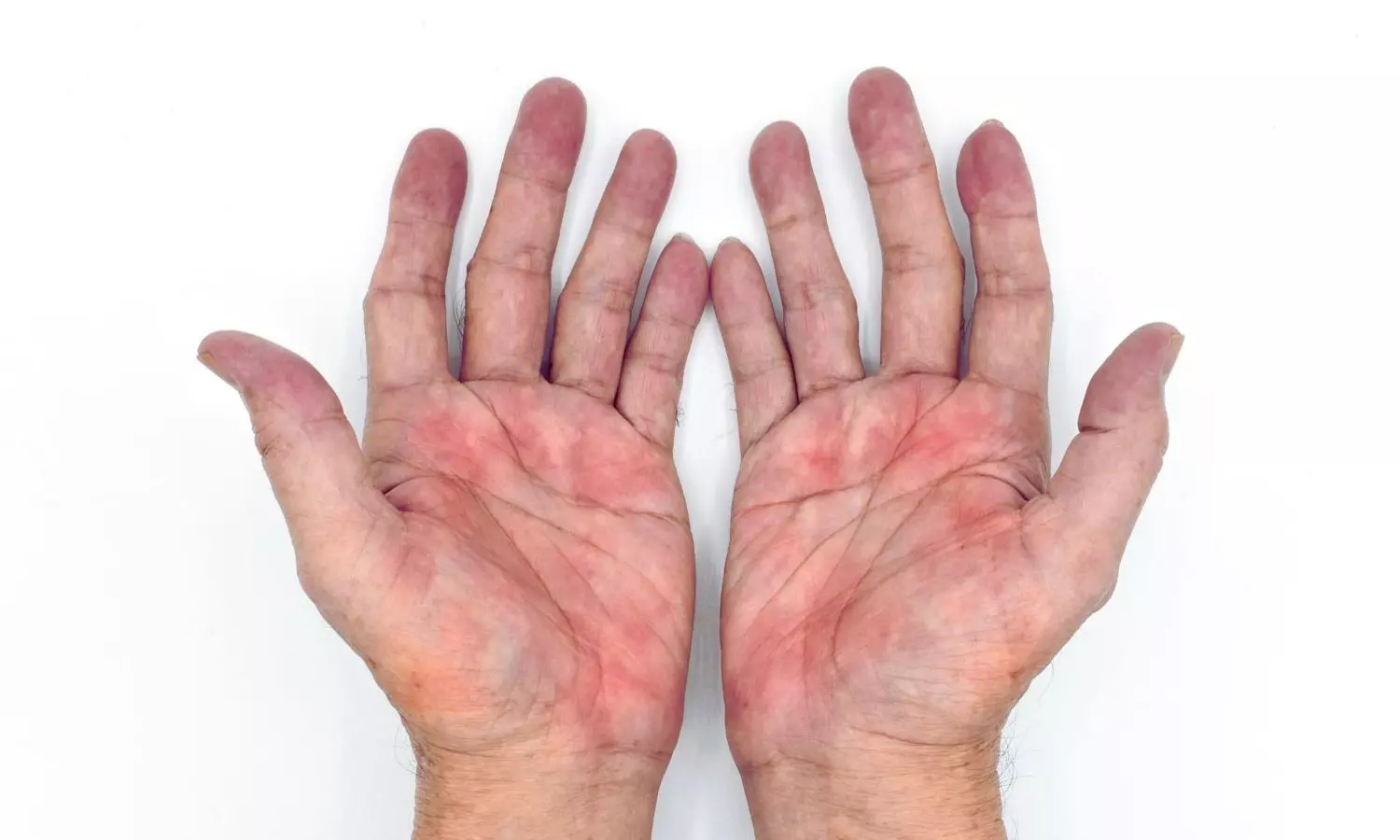
The authors describe the case of a 31-year-old man with severe, generalized atopic dermatitis who was receiving dupilumab injections every two weeks. After a year of treatment, while his overall skin condition had improved, he developed persistent redness, scaling, and painful fissures on his palms, accompanied by intense itching. The condition significantly interfered with his profession as a guitarist.
Extensive evaluation did not suggest contact dermatitis, and patch testing was deemed unnecessary. Microbiological tests showed mixed bacterial growth, while fungal cultures were negative—though this did not rule out Malassezia, which is known to be difficult to culture. Clinically, the presentation did not match other common diagnoses such as psoriasis or dyshidrotic eczema. The patient also had mild facial redness.
Initial management with potent topical corticosteroids provided limited benefit. However, the patient reported some improvement with antifungal creams, particularly miconazole. This response, along with an elevated level of Malassezia-specific immunoglobulin E, raised suspicion of a fungal-related mechanism. Based on this, the clinicians initiated oral fluconazole at a low daily dose.
Within four weeks, the patient experienced notable improvement in his symptoms. However, symptoms worsened soon after discontinuing the medication, prompting its reintroduction. Continued therapy led to sustained improvement, with reduced redness, scaling, and fissuring of the palms over several weeks. The patient also noted improvement in facial redness. Importantly, long-term use of fluconazole was well tolerated, and the patient was able to resume his professional activities.
The authors suggest that fluconazole may work by reducing Malassezia colonization on the skin and through its anti-inflammatory effects. They also note that low-dose fluconazole is relatively affordable and suitable for extended use, making it a practical option in selected cases.
This case underscores the need for clinicians to consider fungal hypersensitivity in patients who develop atypical skin reactions during dupilumab therapy. It also highlights the importance of individualized management strategies and careful clinical assessment in cases that do not respond to conventional treatments.
Reference:
Selvaraj, K. J., & Lee, G. Dupilumab-Associated Palmar Erythema Successfully Treated With Fluconazole. Australasian Journal of Dermatology. https://doi.org/10.1111/ajd.70089
 Suka
0
Suka
0
 Kurang Suka
0
Kurang Suka
0
 Setuju
0
Setuju
0
 Tidak Setuju
0
Tidak Setuju
0
 Bagus
0
Bagus
0
 Berguna
0
Berguna
0
 Hebat
0
Hebat
0