Implantable Living Materials Contain Infection-Sensing Bacteria That Release Therapeutics
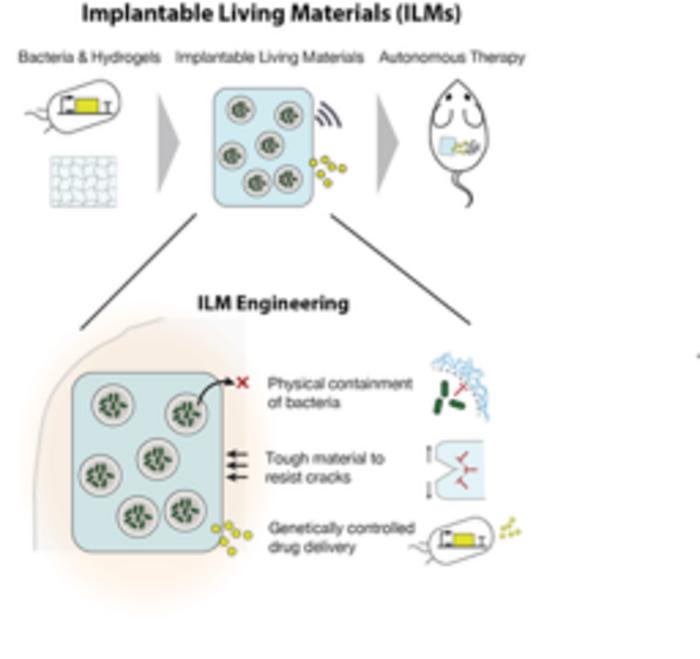
Overcoming a major hurdle in the use of microbes as medicine, researchers at Harvard’s Wyss Institute and John A. Paulson School of Engineering and Applied Sciences (SEAS) have developed an “implantable living materials” (ILMs) platform comprising encapsulated infection-sensing bacteria that can release therapeutic molecules on demand but are kept physically separated from the surrounding tissue.
Wyss Founding Core Faculty member David Mooney, PhD, and colleagues encapsulated a genetically engineered, therapeutic strain of E. coli bacteria within a biomaterial made from a hydrogel that was specifically designed to regulate bacterial growth and resist mechanical stresses, such as those present at physically active sites in the body, demonstrating that the bacteria could be confined for over six months.
To evaluate the material’s clinical potential, the researchers transformed the ILM into an active therapeutic system by engineering the bacteria to detect chemical signals from Pseudomonas aeruginosa, a common cause of implant-related infections. In response to the pathogen, the engineered bacteria autonomously self-destructed to release an antibacterial protein that killed the P. aeruginosa. In a mouse model of joint infection, the system successfully reduced bacterial burden, demonstrating the potential of durable, programmable ILM-based therapeutics for long-term disease treatment. The researchers suggest that their development represents a shift from passive drug depots to autonomous, responsive—and living—therapeutic systems.
“With this new strategy combining both an engineered material with designed mechanical features and genetically engineered microbes that produce therapeutic payloads on demand, we provide a generalizable framework for deploying future microbial medicines,” said Mooney. “The precision, safety, and therapeutic durability afforded by this ILM strategy could be a potential solution for treating a wider range of diseases and infections, enabling therapeutic efficacies that might surpass those of other drug delivery strategies.”
Mooney, the Robert P. Pinkas Professor of Bioengineering at SEAS, is co-senior and corresponding author of the team’s published paper in Science, titled “Implantable living materials autonomously deliver therapeutics using contained engineered bacteria,” in which the authors concluded that their collective results “… establish ILMs as a foundation for deploying microbial medicines in vivo as autonomous therapeutic depots across diverse disease settings.”
Patient recovery from many debilitating conditions and diseases could be sped up significantly and be more effective if drugs and therapeutic molecules were delivered right to where they are needed in the body, over the entire regenerative process, and in doses finely tuned to therapeutic needs. An intriguing way to achieve this is the use of implantable, synthetically engineered, living cells that can sense injury or disease-associated conditions in their environment and flexibly respond by producing the right amount of a therapeutic molecule.
“Synthetically engineered cells are emerging as living therapeutic modalities, capable of sensing physiological conditions and producing bioactive payloads in vivo,” the authors wrote. Unlike conventional drugs, these “living therapeutics” can sustain themselves in vivo and survive in many biological environments, including tumors, inflamed tissues, infected tissues, and even within human cells.
Bacteria are particularly attractive because they can be genetically programmed to release therapeutic molecules in response to specific biological signals. Bacteria can thrive in harsh physiological environments within the body, such as within infected or inflamed tissues, tissues undergoing mechanical movements, and tumors.
Some such microbial therapies have even advanced into clinical trials to treat certain cancers, metabolic disorders, and the progression of kidney stones. However, thus far, such trials have failed, and microbes are feared to also pose significant safety risks because they cannot be contained at specific sites in the body. “… controlling microbial off-target effects remains a key safety consideration because dissemination and associated toxicity have been reported across multiple clinical contexts,” the authors continued.
Previous implantable biomaterial systems, such as hydrogels and capsule-like enclosures, have shown some success in confining microbes, but only for short periods—typically no more than two weeks. “Implantable hydrogels offer a physical strategy to confine therapeutic cells at target sites,” the investigators commented. “Such living materials hold promise as localized drug depots with the capacity to dynamically respond to diseased environments … In this work, we present an implantable material that encapsulates and confines bacteria, wherein synthetically engineered microbes produce therapeutic payloads from within.”
First author Tesuhiro Harimoto, PhD, who spearheaded the project as a postdoctoral fellow in Mooney’s group, explained further, “In the beginning, we asked the seemingly simple question, what if we could design a material that safely encapsulates drug-delivering bacteria inside and allows therapeutic drugs to pass through to where they are needed.” Although scientists have extensively studied how physical parameters of synthetic materials change with tweaks made to their composition and chemical connections, “this was a big ask since the encapsulating material had to reconcile two often contradictory features: it needed to be sufficiently ‘stiff’ so that bacteria pushing against it from the inside can’t break it apart, and sufficiently ‘tough’ to provide a enclosure that protects against external physical stresses in mechanically active tissues.”
![Graphical abstract: "Implantable living materials autonomously deliver therapeutics using contained engineered bacteria" [Tetsuhiro Harimoto]](https://www.genengnews.com/wp-content/uploads/2026/05/low-res-300x282.jpeg)
To realize ILMs, the team started with polyvinyl alcohol (PVA), which is already used clinically, and processed it to form nanoscale interactive crystalline domains. The resulting scaffolds are simultaneously highly stiff and tough. “Finding out how to fabricate optimal hydrogels from PVA that are crosslinked through dense crystalline domains, and how to do this in a way that keeps the enclosed bacteria alive and active, was a big part of our study,” said Harimoto. The researchers included the bacteria in their fabrication process within tiny droplets of gelatin that protected them against desiccation and selective chemical manipulations.
This strategy allowed them to fabricate an ideally stiff and tough material scaffold around the bacteria, using a combination of tolerable freeze-thaw cycles, salt conditions, and chemical treatment times. Late in the process, via a slight shift in temperature, the gelatin microgel could be dissolved to create internal voids for the bacteria to thrive in. Due to the tiny pore sizes within the PVA material, the bacteria remain constrained while the soluble molecules they produce can travel to other sites in the body.
The resulting ILM safely contained the bacteria over extended time intervals of up to six months and was resistant to repeated mechanical stresses. “We developed a hydrogel scaffold with dual mechanical features: high stiffness to regulate bacterial proliferation and high toughness to resist material fracture under physiological stress,” the investigators stated. “This design achieved complete bacterial containment for six months and withstood multiple forms of mechanical loading that otherwise caused catastrophic material failure.”
To provide proof-of-concept for ILMs, the team focused on the infection of implanted periprosthetic devices designed to treat fractures or bone loss around existing artificial joint replacements by pathogenic P. aeruginosa strains. Many treatments with periprosthetic devices fail due to infection, which goes along with inflammation and the spread of antibiotic resistance. “We evaluated the use of ILMs for periprosthetic joint infection in vivo,” they wrote. This model was designed to capture early postimplantation infection during which most infections arise in clinical settings.”
To effectively treat this and other types of infection, the therapy-delivering bacteria within the ILM needed to be genetically engineered to function as a drug depot with autonomous “sense-and-respond” capabilities. To achieve this, the team installed a synthetic gene circuit in the E. coli strain that enabled the bacteria to sense a small diffusible metabolite produced by P. aeruginosa, known as N-acyl homoserine lactone (AHL), and, in response, activate a self-destruction gene to trigger cell lysis. The self-destruction process, triggered in a fraction of ILM bacteria, resulted in release from the ILM of a synthetic P. aeruginosa-killing protein called chimeric pyocin (ChPy) that the bacteria produce continuously. ChPy is toxic to P. aeruginosa, erasing the pathogen in the local ILM environment.
“When we tethered a therapeutic ILM to a stainless steel periprosthetic device that was infected with a pathogenic P. aeruginosa strain isolated from a patient’s wound and implanted next to the femur bone of mice, it significantly reduced the pathogen burden while safely containing its engineered bacteria over a three-day treatment course,” said Harimoto. “In contrast, in mice that we treated with a non-therapeutic control ILM that did not produce ChPy, the numbers of P. aeruginosa bacteria continued to rise over the same time interval. This demonstrated the ability of therapeutic ILMs to autonomously sense and treat periprosthetic infection in vivo.”
The researchers think that specifically engineered ILMs as a novel class of therapeutics with excellent safety features and locally targeted drug release capabilities have broad potential, ranging from tissue regeneration to immune modulation in a variety of disease settings. A patent application describing the use of ILMs for drug delivery has been filed.
In their paper, the authors wrote in summary, “ILMs are distinct from other therapeutic modalities, such as drug-loaded depots and vaccines. By directly sensing pathogen-derived signals and locally releasing antimicrobial payloads, ILMs enable rapid, antigen-independent intervention at the implant site. This localized, autonomous mode of action is well-suited for periprosthetic joint infection, where early intervention is critical.” Their collective results, the team suggests, “…establish ILMs as a foundation for deploying microbial medicines in vivo as autonomous therapeutic depots across diverse disease settings.”
In a related perspective, Kaige Chen, PhD, and Quanyin Hu, PhD, at the School of Pharmacy, University of Wisconsin–Madison, acknowledge that further work will be needed to determine whether contained living therapeutics can function in vivo over long periods. Nevertheless, they said, “The study of Harimoto et al. addresses a central obstacle to deploying living therapeutics—keeping bacteria physically separated from the surrounding tissue. Chen and Hu further note that the in vivo findings in the artificial joint mouse model “… could advance living therapeutics from short-lived proof-of-concept systems to durable, programmable medicines.”
The post Implantable Living Materials Contain Infection-Sensing Bacteria That Release Therapeutics appeared first on GEN - Genetic Engineering and Biotechnology News.
Apa Reaksi Anda?
 Suka
0
Suka
0
 Kurang Suka
0
Kurang Suka
0
 Setuju
0
Setuju
0
 Tidak Setuju
0
Tidak Setuju
0
 Bagus
0
Bagus
0
 Berguna
0
Berguna
0
 Hebat
0
Hebat
0